Continuous
non-invasive
hemodynamics
Watch our video
Continuous
non-invasive
hemodynamics
The Finapres® NOVA is an innovative hemodynamic monitoring system.
It provides accurate non-invasive continuous blood pressure monitoring using just a finger cuff!
Application Fields
Beat-to-beat hemodynamics
Finapres devices apply in the fields of Autonomic Failure Diagnosis, Hemodynamic Evaluation, Education, and other application fields.
Application Fields
Beat-to-beat hemodynamics
Finapres devices apply in the fields of Autonomic Failure Diagnosis, Hemodynamic Evaluation, Education, and other…-
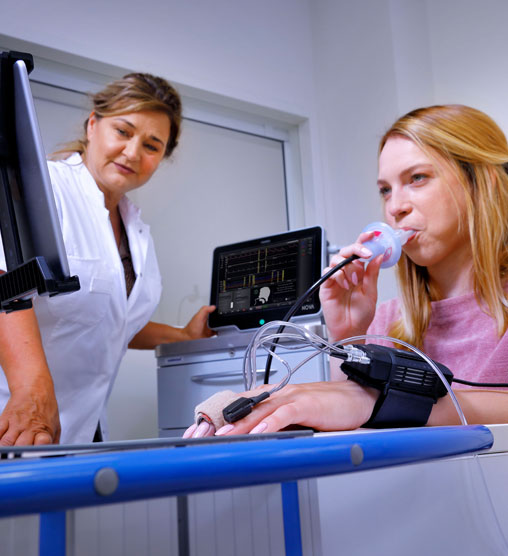
Other application fields
Orthostatic Hypotension, Space Flight, Sleep Disorder, and Pharmacological Research.
Read More